Dr Annabelle Leong is an Ear, Nose and Throat (ENT) surgeon with fifteen years of ENT experience, having trained and worked in the United Kingdom, Canada and Singapore. She manages all types of ENT conditions, including nasal, sinus and sleep disorders in both adults and children. She has subspecialty interests in hearing disorders, and paediatric ENT, having trained at Great Ormond Street hospital, Evelina children's hospital at St Thomas's and the Hospital for Sick Children in Toronto. She is a mother of 2 young sons so she knows exactly what concerned parents go through when their child falls ill.
Ear, nose, and throat (ENT) problems are extremely common in children, including ear infections, blocked and stuffy nose, tonsillitis, snoring and sleep-related breathing issues.
The challenge is to diagnose these correctly in children who may not always be able to report their symptoms. With the right diagnosis, ENT conditions in children can be treated successfully.
Dr Annabelle answered questions from readers on:
- Common ENT problems in children
- Allergic Rhinitis, Chronic Sore Throat, Hearing loss, Nose Bleeds, etc
- Childhood ENT Disorder
- When to see a specialist for these conditions
- Causes of these problems
- Treatment options in Singapore
- Treatment costs in Singapore
Is snoring in children indicative of a medical problem?
Snoring in children is quite common but in about 10% of children who snore, this may be a sign of underlying airway obstruction leading to problems with sleep-related breathing or obstructive sleep apnea (OSA).
OSA in children is mostly caused by enlarged tonsils and adenoids but suffering from a blocked nose due to allergy problems may worsen the breathing when asleep. The concern with OSA in children is that it prevents them from getting good quality sleep, which in turn, affects their general wellbeing, as well as their mental, emotional and behavioural development, possibly even impairing their academic performance.
How can I tell if my child has an ear infection?
It may not always be easy to tell if your child might be suffering from an ear infection, especially if they aren’t able to speak properly yet.
But the parents of my kiddie patients with ear infections have told me that they were worried about their child tugging repeatedly at his or her own ears, or trying to stick their fingers into their ears, so that was why they brought their child to see me for a thorough checkup.
What happens if my child keeps getting ear infections?
When you say your son was diagnosed with a middle ear infection, this usually means that he had an infection of his eardrum with possibly some infected fluid trapped behind. If a short course of antibiotics doesn’t help, then the usual treatment is to have a tiny ventilation tube called a “grommet”, inserted into the eardrum to improve the ventilation of the middle ear.
Can my child lose hearing from an ear infection?
Whether your child is at risk of permanent loss of hearing with recurrent ear infections, really depends on what part of his ear keeps on becoming infected. If it is the outer ear canal which becomes infected, then any swelling of the skin will temporarily block his ear and lead to hearing loss but this usually returns once the outer ear infection resolves.
The real worry though is that recurrent ear infections leading to a buildup of pus (frank infected yellow liquid behind the eardrum, see picture below) can potentially spread to the inner ear where the delicate hearing organ (cochlea) lies.
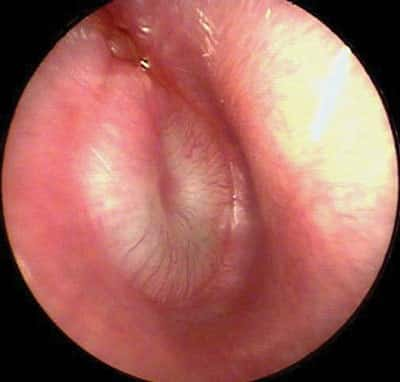
How to prevent ear infections when my child swims?
Swimming to prevent swimmer’s ear! Swimmer’s ear occurs when water enters the ear canal and irritates the delicate ear skin, giving rise to an ear infection (otitis externa).
This can be quite painful and uncomfortable as the ear may feel blocked. We usually treat swimmer’s ear by cleaning the ear out carefully and applying some antibacterial ointment inside or prescribe some eardrops.
Can ear infections in children be prevented?
Yes, there are. The most important first step is not to dig your child’s earswith anything, including cotton buds, as this may accidentally injure the delicate skin inside or puncture the eardrum, which could lead to a permanent hearing loss. The earwax inside your child’s ears contains natural oils to keep the skin moisturized and healthy.
How is Sinusitis in children treated in Singapore?
rue sinusitis or sinus infections are not that common in children actually as the sinuses are not fully developed until late teen years. The sinuses are normally air-filled spaces in the skull.
Children with sinus infections may present with a “cold” lasting for 10-14 days, with yellow nasal secretions, pain over the cheeks or between the eyes, fever and blocked nose.
How does one differentiate sinusitis from a cold in a child?
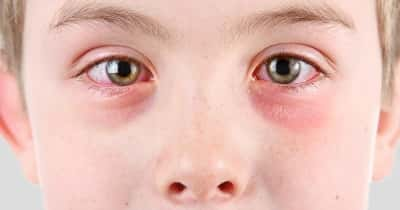
It is not always easy to tell the difference between a common cold and sinusitis. But from experience with my paediatric patients, these are typically the symptoms to watch out for:
- if the cold lasts an unusually long time such as more than 10 days
- thick yellow-green nasal mucus
- puffy swollen eyes (see picture above)
How do I know what causes hay fever in my child?
Yes, it is definitely worth having an allergy test to identify the triggers of your daughter’s hayfever. Not only can you then learn to avoid the triggers once they are known, but there are now also newer forms of treatment for certain triggers such as grass and house dust mite which aim for a permanent cure to desensitise the immune response against these triggers.
What is the relationship between allergic rhinitis and asthma?
Many of my paediatric patients suffer from both asthma and allergic rhinitis. Asthma is a hyper-reactive inflammatory narrowing and obstruction of the lower airways of the lung, which causes recurrent wheezing, difficulty breathing, chest tightness and cough.
Should I remove earwax from my child’s ears?
You don’t actually have to do anything to get rid of the earwax in your son’s ears. Earwax contains protective natural oils to moisturize the delicate skin of the ear canal. So it is all right to have some earwax in your son’s ears.
In fact, having ears which are “too clean” may lead to the ear feeling dry and itchy.
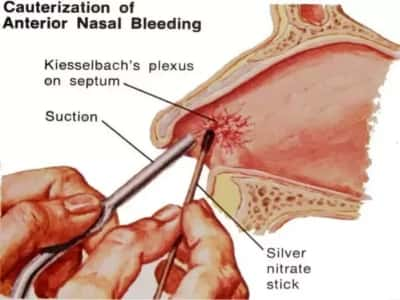
Is nosebleeds in children a sign of something serious?
Nosebleeds are quite common in children. We see many children at our clinic with this problem and sometimes, it is related to hayfever with recurrent sneezing irritating the delicate lining of the nose, the prolonged use of nasal steroid sprays or simple digging of the nose.
How can I find the best ENT doctor for my child in Singapore?
Although this question is subjective, I actually find it easy to answer!
You should select the ENT doctor who is very experienced in dealing with children of all ages and can build up a totally comfortable rapport with both your child and yourself to set your whole family at ease.
What could cause a white lump on the tonsil in someone with recurrent throat infections?
From your photo, that white lump on your left tonsil looks like a mucous cyst (collection of trapped secretions from your tonsil glands). It may also be a tonsil stone.
Both these conditions are commonly seen in people who suffer recurrent episodes of tonsil infections, such as yourself.
The fact that you have suffered from nasty tonsil infections for so many years puzzles me as to why you have chosen to continue to do so, when there is a relatively straightforward solution: …
What are possible causes of a growing lump on the tonsil?
In view of its enlarging size and the fact that is is just on one side, I would strongly advise you to have it thoroughly checked out by an ENT specialist.
Rarely, tonsil lumps may turn out to be more sinister in nature, such as lymphoma (lymph gland cancer) or squamous cell cancer (linked to smoking and Human Papilloma Virus exposure).
Why is my nose always blocked on one side?
Ideally, you would need a proper examination of the inside of your nose with a flexible nasal endoscope to check if the main central bone in your nose might be crooked or deviated (deviated nasal septum). This is a safe, short and painless procedure we do very frequently at our clinic.
We also need to make sure that …
What non-surgical methods are there to remove a neck cyst? (photo)
The simple answer is unfortunately, there is no non-surgical method to treat these cysts. They are skin cysts which are called sebaceous cysts.
They originate from skin glands which secrete sebum to moisturise the skin but if their drainage outlet becomes blocked, then a cyst forms with a risk of becoming infected like your mum’s.
How do I know if my 1 year old child has a tongue tie or lip tie, and can it be treated?
Tongue ties are pretty common: basically they are bands of soft tissue which tether the tongue down to the floor of the mouth.
They don’t usually cause much of a problem but if they do, then the baby may have some problems feeding/breastfeeding, or the younger child may have a slight speech impediment in the form of a lisp or difficulty pronouncing certain consonants which require the tongue to extend forwards.
Why do I get recurrent sores inside my nose?
In winter, the dry temperate weather can irritate and inflame the delicate lining of the nose which can then break out into sores and blisters.
If you suffer from allergy problems with your nose, that makes it even more sensitive to changes in temperature and humidity.
The simple solution is usually to apply some antiseptic ointment as a barrier to protect the nasal lining.
How do doctors treat a Cobblestone Throat?
Thanks for your question about cobblestone throat. I presume you know what that means but just for everyone out there, the cobblestone throat is used as an appearance of the back of your throat due to the enlarged areas of lymph gland tissue (follicles).
What can I do about a constant running nose?

These are most likely signs of underlying irritation of a hypersensitive nose, a condition termed rhinitis.
The actual cause of rhinitis can range from allergic reactions to substances in the environment such as house dust mite, grass and pollen, to more nonspecific triggers like changes in temperature and humidity.
The nose is a fantastically complex organ designed to react to changes happening around it so it usually produces a certain amount of secretions in normal healthy people anyway.
How can one improve non-stop coughing that is due to cancer treatment?
Thanks for your query re your dad’s persistent coughing after having had Y90 treatment for liver cancer.
Persistent cough as a condition itself has many causes eg postnasal drip due to allergy and sinus problems or acid reflux irritating the voicebox and throat.
However, in your dad’s case, as Y90 involves the introduction of tiny radioactive spheres into the blood supply of the liver tumour, the persistent cough may be related to the side effects of Y90 therapy, as it may lead to radiation pneumonitis
When does a doctor decide to perform a nasal endoscopy for sore throats?
A nasal endoscopy is the most important workhorse of my specialty Otolaryngology (Ear Nose Throat).
We use it to carefully and thoroughly examine all openings of the ear, nose and throat as many pertinent findings may be missed from a mere glance on the outside.
What could be the cause of throat bumps? (photo)
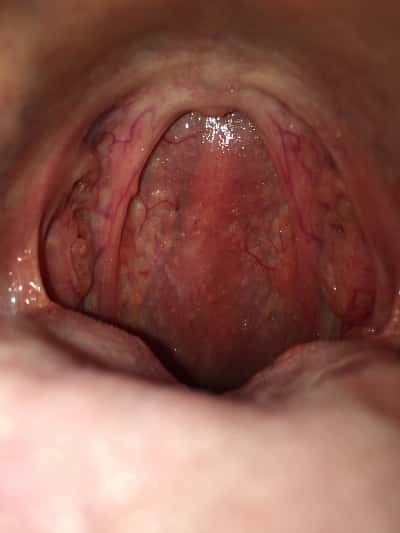
Those little bumps all over the back of your throat are actually lymphoid follicles which are part of the immune system. “Lymph glands” are probably what some people would call them.
Their function is to drain the fluid from the throat and nose and tongue region so that your immune cells in these lymphoid follicles can screen for infection to help make the specific antibodies when necessary.
You don’t need to worry about them. They may sometimes even appear larger or more inflamed if you come down with a bad cold or the flu.
Why does my toddler keep covering his ears, and could it be a sign of ear infection?
It is quite common to notice your toddler covering his or her ears and it is usually nothing to worry much about.
The top reason for little kids to do this is because they feel overly stimulated by too much sound or loud noises. Pretty much what we would do too as adults if we heard irritating or loud sounds around us. So it is a sort of protective reflex.
The next most common reason is that they may feel scared and this may represent an emotional reaction to what is going on around them.
How to treat sleep apnea without CPAP or surgery?
When you say that your mum can’t tolerate wearing a CPAP mask, I hope she has had the experience of already trying different types of CPAP masks because they come in all shapes and sizes, not just full facial masks which many patients find difficult to tolerate for the whole night.
CPAP masks also come in the form of small neat-looking nasal masks and even nasal specs/tiny tubes sitting just at the nostril area.
Other options of treating obstructive sleep apnea also include wearing a specially fitted dental appliance in the mouth, called a Mandibular Advancement Device (MAD), which looks very much like a retainer people wear when they have braces fitted.
How are sinus headaches differentiated from other headaches?
Headaches can be pretty painful and can really affect your husband’s quality of life!

Before we assume though that sinus problems are causing his headaches, we would usually take a detailed history to find out the location and pattern of the headaches as well as other associated symptoms like blocked or a runny nose, a colour of his nasal discharge, any nausea or vomiting, vision problems.
What is the link between nasal polyps and sinus issues?
Nasal polyps are usually benign inflammatory growths which arise from the thickened lining of your sinuses.
As the nasal polyps grow larger, they start to block off the openings of the sinuses, preventing from draining properly and resulting in the trapping of thick mucus inside the sinuses.
Bacteria and viruses can easily grow in these pools of mucus, leading to frequent infections of the sinuses, so that you suffer:
- headaches
- blocked and runny nose
- smelly yellow/greenish nasal discharge
- postnasal drip causing you to cough and clear your throat constantly
Could prolonged hoarseness be a sign of throat cancer?
I think that your dad should most definitely have his hoarse voice checked out to make sure it isn’t due to a more worrying cause like cancer.
I always advise anyone who has had a persistent hoarse voice for longer than 2 weeks to undergo a thorough checkup, even if he is a non-smoker.
Anyone with a hoarse voice who smokes or is an ex-smoker should not hesitate to have their throat and voicebox examined carefully as the chances of cancer or pre-cancer changes are much higher than in a non-smoker.
How does TMJ affect the balance system and cause dizziness?
One of the lesser known symptoms of Temporomandibular Joint Dysfunction (TMJ/TMD) is dizziness as your TMJ or jaw joint sits very close to the structures of the middle and inner ear. Your TMJ is supplied by a rich network of nerves which also supply different parts of the ear itself.
So if there is any irritation or inflammation around the TMJ, then it may potentially affect the ear and give rise to ear-related symptoms such as:
- ear pain
- tinnitus (noise in ear)
What is the normal progression of an ear infection, and when should I seek help?

Eardrum infections commonly result from having had a bad cold or flu as the same "bug" that caused the flu, tracks up the pressure tubes (Eustachian tubes) which lead to your eardrums.
I wonder what antibiotic you have been prescribed? The "bugs" which cause ear infections may sometimes be resistant to simple penicillin/amoxicillin which is what many family practitioners usually prescribe.
I hope you're on Augmentin or Klacid because they are the best antibiotics for eardrum infections.
How is vertigo diagnosed and treated in Singapore?
Vertigo isn't a diagnosis but actually just a word used to describe a symptom of feeling as if the whole room and the objects inside it are spinning or moving round and round. It can certainly make you feel like vomiting!
The fact that your vertigo becomes worse when you change position, suggests that it is more likely to be due to an inner ear problem, which we call "peripheral" in the ENT world, instead of "central" which refers more to abnormalities involving the brain.
Can the flu cause ear pain and a toothache?
Yes, indeed, your ear pain and toothache may be related to your flu.
As Dr Jaclyn, my dental colleague, has rightly described in her answer, this may be due to referred pain where the same group of nerves is supplying surrounding structures because the flu "bug" is causing inflammation and irritation of the lining of your sinuses, teeth and the eardrum.
However, ear pain and fever may also be due to an actual ear infection so it is important to examine the ear carefully to check for any redness, swelling or even infected fluid/pus trapped behind the eardrum.
What is this wart like swelling in my throat? (photo)
In your photos, there appears to be a small swelling on your right tonsil. It looks like it is probably benign although the only definitive way to tell for sure is to remove it and send it off for analysis. This is even more important if you smoke.
HPV (Human Papilloma Virus), of which there are 4 subtypes which are usually sexually transmitted, may cause warts or papillomas, or even more worrying conditions like cancer but there is no way to say for sure that HPV is the cause of this swelling unless we remove it and run some tests.
What should I do next if I still have green phlegm and cough after completing my course of antibiotics?
If you're still coughing with thick green phlegm even after a course of antibiotics, then you definitely should get your nose and sinuses carefully examined by your friendly ENT specialist who can insert a flexible tiny endoscope/camera into your nose to take a look.
I would say that this is one of the more common problems that patients come to see me for, with many patients already having been seen by their Respiratory/Chest specialist.
How can I prevent frequent sinus infections?

We see so many patients at our clinic with the same set of symptoms just like yours!
They typically suffer from:
- a blocked and runny nose
- yellowish nasal discharge
- headaches and facial pain, and can be rather unwell with fever too
If you come down with a sinus infection, you will very likely need to be prescribed a course of strong antibiotics to prevent it from spreading further, as sinus infections have the potential to involve the eye or even the brain, although these events are fortunately rare.
What could be the cause of a white patch inside the ear? (photo)
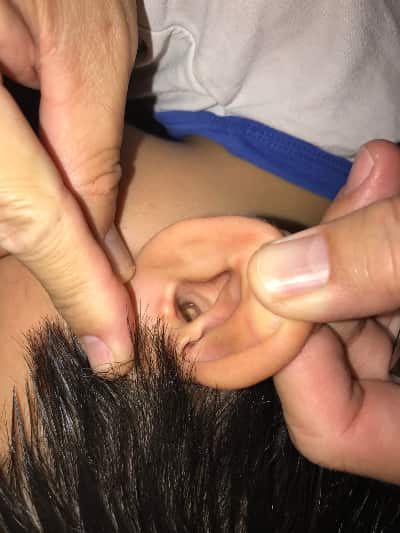
I looked closely at your photo but I wonder which "patch" you're referring to?
There is a very tiny whitish speck just inside the opening of the ear which really looks just like a bit of flaky dry skin, probably nothing to worry about.
However, deeper in the ear, there appears to be a larger area of whitish scaly-looking plaque which might be sitting very close to or on the eardrum itself.
Is it possible to recover from hearing loss that happened many years ago?
Sudden hearing loss is regarded as an "ENT emergency" i.e. if you lose your hearing suddenly, you should seek medical help as soon as you can so that appropriate medications may be started as early as possible to maximise the chances of hearing recovery.
Frankly speaking, the best chances for recovery of her hearing would have been within the first 72 hours, with many patients noticing that the peak time of recovery is within the first 2 weeks after having lost their hearing suddenly.
Many ENT doctors will treat with medications up to the 6 week window: After this window, the chances of recovery begin to fall drastically.
Ever wanted to ask a health question to a specific renowned specialist in Singapore? Human Sessions are when these expert doctors answer all your questions!
View the complete list of upcoming Human Sessions here.







