There are days when our gut just doesn’t agree with us. We’ve all experienced diarrhoea and constipation at some point in our lives, but when does it require medical attention? In Singapore, about 4% of the population suffers from Irritable Bowel Syndrome (IBS), which can occur in the form of abdominal bloating, pain, diarrhoea or constipation.
The symptoms of irritable bowel syndrome could start as early as childhood [1] and is commonly experienced among adults too. In fact, IBS is the 2nd highest cause of work absenteeism, right after the common cold. Unfortunately for some, IBS can be a long-term problem and can negatively impact their everyday life. Read on as Dr Tan Chi Chiu walks us through all we need to know about IBS, how to best manage it and when to seek help early.
What is Irritable Bowel Syndrome?
IBS is a functional gastrointestinal disorder that affects the digestive tract. It is characterised by abdominal pain and altered bowel habits [2] that lack specific and unique organic pathology. This means that its exact cause is unknown, but commonly linked to oversensitive nerves in the gut, stress or genetic predisposition.
Other terms for IBS include:
- Spastic colon
- Irritable colon
- Nervous colon
There are three clinical subtypes of IBS: [3]
- IBS-D (Diarrhoea predominant)
- IBS-C (Constipation predominant)
- IBS-M (Mixed diarrhoea and constipation)
Table: IBS Subtypes based on Stool Consistency as per the Bristol Stool Scale
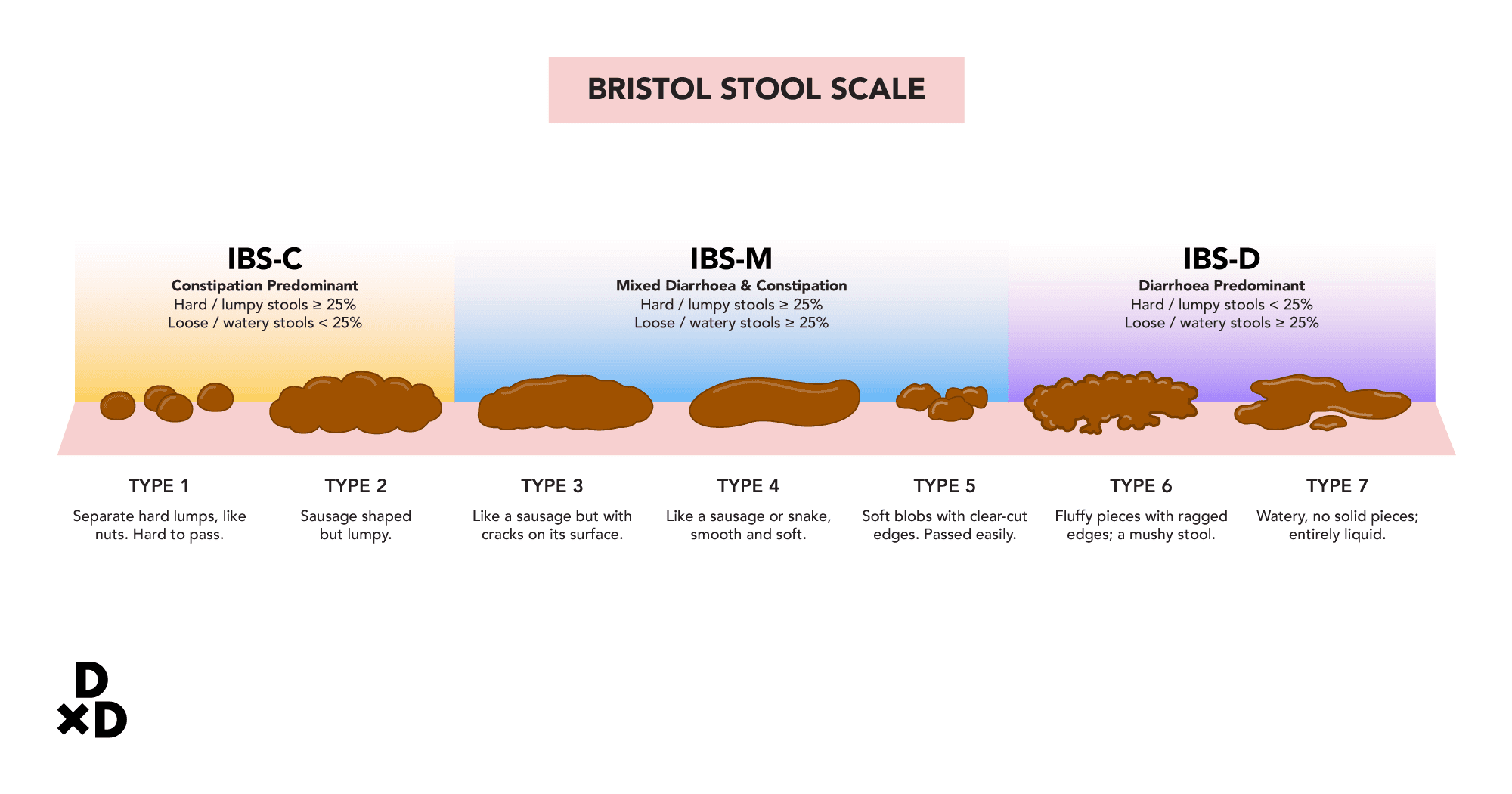
Patients may experience a change in subtypes, as frequently noted by doctors.

Some common signs and symptoms of IBS include:
- Mucorrhoea — mucus in the stool [4]
- Abdominal bloating
- Subjective distension — due to bloating
- Objective distension — measurable increase in abdominal girth
- Flatulence (Farting)
- Tiredness and lack of energy
- Backache
- Problems with peeing — needed to pee often, sudden urges to pee, feeling as though you cannot fully empty your bladder
- Incontinence — not being able to control your pooping
- Unusual bowel movement — altered stool frequency, appearance or urgency
Read also: What is the difference between IBS and gastritis?
When should I consult a doctor for IBS?
If symptoms are severe, persistent, recurrent or affect your quality of life, it would be good to consult a doctor for proper diagnosis and treatment.
There are some red flags or alarm symptoms that may prompt you to seek help: [5]
- Rectal bleeding
- Unexplained weight loss (>10% over 3 months)
- Unexplained iron deficiency or anaemia
- Nocturnal symptoms — e.g. diarrhoea at night
- Fever
- Laboratory abnormalities such as inflammatory markers or electrolyte disturbances
- Family history of colon cancer, colorectal cancer, or allergy to gluten
It is important to take note of these urgent symptoms as they could be underlying signs of a more serious condition like Inflammatory Bowel Disease (IBD). IBS is a functional disease, whereas IBD is a structural disease, involving inflammation of the large bowel (Ulcerative Colitis) or anywhere along the digestive tract (Crohn’s Disease) [6] — which means that the symptoms you experience are caused by physical damage to your digestive tract, such as bleeding or ulcers. If left untreated, it could lead to further damage of the digestive tract or even colon cancer if the colon has been inflamed for many years.
If there is a concern about the possibility of Inflammatory Bowel Disease or IBD, it is paramount that you consult a doctor in order to run tests to diagnose whether IBD is present and to discern what form of IBD you have and to ensure that you receive proper treatment. Some of these tests include a stool test, CT or MRI scans, gastroscopy and/or a colonoscopy.
Read also: For younger patients in their 20s and 30s, should they go for a colonoscopy or CT scan if their “IBS” is bad?
What causes Irritable Bowel Syndrome?
It is not entirely clear what causes IBS because there are no specific pathologies. Medically, it is likely a combination of endogenous factors (within the person and localised factors in the gut) and environmental factors. Such factors include:
- Microbial composition of the gut
- Metabolites
- Immune function
- Stress and anxiety
- Inflammation in the gut [2]
High stress and anxiety - It is known in the gut-brain model that the brain and gut are connected by nerves. [7] Hence, any cognitive effects by the brain can also affect the digestive tract. This is also why those with high stress and anxiety can have IBS. Conversely, IBS might also make you more worried and anxious, creating a vicious cycle with reinforcing effects. [5]
Microbial composition of the gut - changes in your gastrointestinal tract’s natural microbiome (the bacterial composition that is normally found in your gut) could lead to IBS.
Immune function - IBS can be caused by nonspecific causes or a surplus of bacteria in the small intestines (bacterial overgrowth). However, technically speaking, if an infective or inflammatory cause can be proven, then it isn’t really IBS. The possibility remains however, that IBS can be related to subtle inflammatory changes that are hard to prove. There is a well known association between gastroenteritis and subsequent IBS symptoms. This suggests that an inflammatory insult to the bowels may precipitate IBS.
It may also be helpful to note that the other risk factors for IBS are age, genetic disposition, food sensitivity and certain medications. Women are also twice as likely to have the condition — although the reason for this is unclear, research suggests it may be caused by the changing hormones in the menstrual cycle.
What foods can trigger Irritable Bowel Syndrome?
In general, there isn’t a specific list of foods that we would advise you to refrain from eating. However, there is evidence that some patients can be helped by reducing their intake of high-fibre foods like beans.

Milk and dairy products should also be avoided where it is likely that you are lactose intolerant, or you can opt for lactose-free milk instead.
Gluten sensitivity may also affect IBS, although the research in this area is currently inconclusive. It is important to note that gluten sensitivity is not the same as Coeliac Disease, in which gluten provokes an allergic antibody response that attacks the absorptive lining of the small intestine. Gluten sensitivity is difficult to prove as there are no biomarkers.
Also read: What is the difference between gluten sensitivity and celiac disease?
Some recommend avoiding FODMAP foods, the acronym being for Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols.These are short-chain carbohydrates and sugar alcohols that are poorly absorbed by the body, which could result in abdominal pain and bloating. [8] FODMAPs occur in some foods naturally or as additives. However, they are found in so many kinds of food that it is almost impossible realistically to avoid all of them for long periods.
Although tedious, people with IBS could try avoiding all the different FODMAP foods and then (assuming that the symptoms actually resolve) by adding them back one by one, through the process of elimination, see how their gut reacts to each type of food item. Perhaps this could help them understand their food sensitivity and which specific foods aggravate their IBS symptoms.
Read also: What diet do doctors recommend for irritable bowel syndrome with constipation (IBS-C)?
Will Irritable Bowel Syndrome go away on its own?
IBS could go away on its own, although the reason for that is unclear as so many factors come into play. It could be that your circumstances have changed, such as eating habits or other resolved environmental factors such as reduced stress and anxiety.
There are cases where IBS can be chronic, recurring over months and years, or going on and off repeatedly.
How is IBS diagnosed? What is the first consultation like?
To diagnose IBS is tricky, but coming prepared with a detailed history of your symptoms and food habits would greatly help the doctor. It may also be useful to keep a “food and symptom” diary, where you can keep track of your food intake and symptoms, making it easier to investigate the condition and discern whether you have any food sensitivities.
After detailed history taking, a full clinical examination in the clinic is usually conducted to look for evidence of any obvious disease. This could include a rectal examination. If deemed appropriate, some simple tests could be done, such as a blood panel or stool tests to rule out any specific illnesses. [9]
If it is quite clear from the clinical history, examination and basic tests that IBS is the culprit, then no further testing is required.
Should the history, examination or initial investigations suggest that there may be other underlying factors, or the patient is older, perhaps over 40 years, and more at risk of serious illnesses, we may carry out further testing such as:
- Imaging tests e.g. Ultrasound, CT or MRI scans
- Gastroscopy and/or colonoscopy
Read also: How do doctors diagnose IBS, and which health professional should I see in Singapore?
What are the treatment options for IBS?
It is imperative to come to a definite diagnosis of IBS and not leave patients with a sense that the doctor isn’t sure of the diagnosis, or that there is a high chance of another diagnosis being missed.
Confidence building is very important and the first requirement is a very good patient-doctor relationship. Education and reassurance from the doctor can go a long way in managing IBS. Patients will be informed that IBS is a chronic disease but there are many ways of managing it and it is not hopeless.
Initially, simple measures such as changing dietary habits, acknowledging stressors and learning how to manage them may be sufficient to reduce symptoms. If symptoms are more severe, medicines are also available to help.
Mild Symptoms
For mild symptoms, the doctor may want you to make some dietary adjustments in some of the ways stated below:
- Exclude gas-producing foods e.g. beans, onions, celery, carrots, raisins etc.
- Avoid lactose — IBS may be due to lactose intolerance or sensitivity to other components in milk
- Low FODMAPs diet — in this case, you may need to consult a dietician [10]
There is limited evidence to show that avoiding gluten can help in IBS, although a genuine gluten sensitivity should be considered.
Physical activity is advised, as studies have shown that 20 to 60 minutes of moderate to vigorous activity 3 to 5 days a week have a positive effect on IBS patients.
Moderate to severe symptoms
For moderate symptoms, certain drug treatments (pharmacological therapy) in the following categories will be necessary: [11]
- For constipation (IBS-C)
- Laxatives
- 5-HT4 receptor antagonists
- Calcium channel activators
- Guanylate cyclase antagonists
- For diarrhoea (IBS-D)
- Antidiarrheal agents
- Bile salt sequestrants
- 5-hydroxytryptamine-3 (serotonin) receptor antagonists
- For abdominal pain and bloating
- Antispasmodic agents
- Antidepressants
Antibiotics and probiotics are not routinely recommended. Probiotics only have modest and inconsistent benefits, although they are associated with symptom improvements.
Read also: Would you, as a doctor, recommend probiotics for irritable bowel syndrome (IBS), and why?
Severe symptoms
In severe cases, stronger medicines can be prescribed. More sophisticated follow-up tests such as more imaging tests, tests for small bowel bacterial overgrowth (SIBO) or malabsorption of various sugar molecules may be conducted where necessary for intractable symptoms.
In some cases, meditation or cognitive behavioural therapy from counsellors or psychologists as a form of treatment may be introduced to curb severe stress and anxiety. [10] In extreme cases, a referral to a psychiatrist may be necessary.
Read also: How Mindful Breathing Helps Reduce Stress

Are there any alternative treatments or home remedies for IBS?
Home remedies have a “soft” therapeutic effect. Mint or ginger tea and peppermint oil can calm the digestive system, so it is good to take them after meals, especially for symptoms of indigestion after food.
If the symptoms are mild enough that they can be soothed by tea or other home remedies, then, by all means, take them! Many patients find that chamomile tea helps calm their nerves, which in turn, helps calm their digestive system as well.
Yoghurt is a good source of probiotics and would make a good alternative for milk if you are sensitive to lactose in milk. Other alternatives for dairy beverages would be nut milks.
It is also perfectly fine to avoid certain foods that you have self-identified as triggers to bloating or distention.
Read also: How do probiotics benefit gut flora and promote colon health?
Are there any misconceptions about Irritable Bowel Syndrome?
- IBS is not a failure of diagnosis of other symptoms — the diagnosis given is a concrete one and not due to failure to find the real diagnosis through investigations.
- IBS is not all in the mind — the symptoms are real and doctors should validate the patient’s perception of the symptoms rather than downplay them as something that is “all in the mind”.
- IBS is not all caused by allergies to food — food sensitivities may play a role but it is not necessarily due to allergies.
- IBS is not all caused by stress — Not all patients who are stressed and anxious will develop IBS, and it is not true to say that you can get rid of IBS once you sort out your stressors.
Summary
Generally, a diagnosis of IBS carries both good news and not-so-good news. The good news is that it is a benign, if irritating condition and except for affecting the quality of life, it never materially harms a patient’s health and will not, in and of itself, lead to any fatal consequences.
The less-good news is that due to the vague and multifactorial nature of IBS, it can sometimes be difficult to find the right combination of interventions, drug or non-drug, to help patients. Patience may be required as your doctor tries his best to manage IBS successfully and there may need to make adjustments in management over time to achieve the best results.
In general, we would advise our patients to maintain an active, physical lifestyle to prevent IBS. Understandably, chronic IBS can be frustrating, but healthy eating habits along with regular exercise can go a long way in helping manage and prevent IBS symptoms. Additionally, managing your stress by various coping measures could also work wonders in alleviating chronic conditions like IBS.
That said, do seek help if you feel that the symptoms are beyond your control or cause you distress. With the right treatment and dietary adjustments, you may be on your way to a better, healthier life. You should certainly seek medical help if you have any of the “red flags” or “alarm symptoms” mentioned above.
You may read more about the topic of gastroenterology here. We have an array of gastroenterology-related articles and questions that will definitely interest you.













