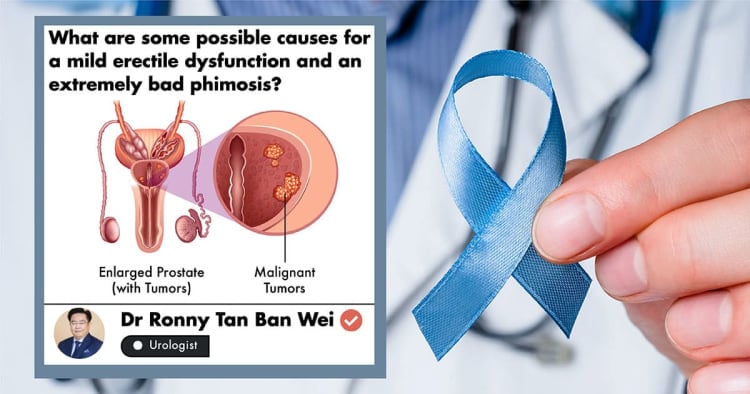
What is Intestinal Cancer?
Intestinal cancer is a type of cancer that is found in your small intestine. It happens when malignant or cancer cells start to form in the tissues of our small intestine [1].
To better understand what is intestinal cancer, it is important to understand how the small intestine works.
The small intestine connects our stomach to our large intestine. It is made up of 3 parts [2],[3]:
- The Duodenum — this is the first and shortest part of the small intestine that is closest to the stomach
- The Jejunum — this is the middle part of the small intestine.
- The Ileum — this is the final and longest part of the small intestine that connects to the large intestine.
Together with other parts of the digestive system (i.e mouth, esophagus, stomach, and large intestine), the small intestine helps to break down food and absorb nutrients that are required for our body [1].
Although the small intestine is the longest and largest part of our digestive tract, cancers in the small intestine are very rare as compared to cancers in other parts of our digestive tract (e.g. colon cancer, rectal cancer, stomach cancer, etc).
What are the types of Intestinal Cancer?
In total, there are 4 main types of intestinal cancer. They are [1] :
- Adenocarcinoma
- Sarcoma
- Carcinoid Tumours
- Lymphoma
Adenocarcinoma
This is the most common type of intestinal cancer — it accounts for 1 in 3 cases of intestinal cancers [1]. Adenocarcinoma usually occurs in the Duodenum or Jejunum part of the small intestine and it starts in the epithelial cells that line the inside of the small intestine.
Sarcoma
Sarcoma occurs mostly in the ileum — the part nearest to the large intestine. The most common type of Sarcoma is known as Gastrointestinal Stromal Tumours (GISTs), a tumor that emerges from the muscle cells of our small intestine [3].
Carcinoid Tumours
Also known as a Neuroendocrine tumour, these tumours are the most common type of small intestine tumour and they are usually slow growing. [1].
Lymphomas
Lymphomas are cancers that start in cells known as lymphocytes — white blood cells found in the blood and lymph tissue [4]. These cancers are usually formed in the Jejunum or Ileum and are commonly Non-Hodgkin Lymphoma.
What are the symptoms of intestinal Cancer?
Unfortunately, in its early stages, intestinal cancer does not manifest itself with specific symptoms or there may even be no symptoms at all. Most intestinal cancers are diagnosed during the more advanced stages.
Should you be classified as an individual with a high risk of having intestinal cancer or have a family history of cancer, it is paramount that you go for frequent screenings to allow for early detection.
If you are suffering from intestinal cancer, the signs and symptoms below may present themselves [5]:
- Blood in stools
- Dark-colored stools
- Unexplained weight loss
- A lump in your abdomen
- Feelings of pain, cramps or swelling in the abdomen
- Anemia — low counts of red blood cell
- Fatigue
- Nausea and Vomiting
The first symptom is often inconsistent pain in the abdomen area. For example, the pain may be triggered or worsened after you eat [6].

These symptoms are not a hard and fast rule and you may experience one without the other. However, do check with your doctor if you are worried or suspect that you may suffer from intestinal cancer for a proper diagnosis.
What causes Intestinal Cancer?
The causes and risk factors for most intestinal cancer are still widely unknown. However, below are some factors that may increase your risk of intestinal cancer.
Demographic Factors
Intestinal cancer is most common amongst people in the older age group, specifically over the age of 50 and the risk increases with age [2].
Lifestyle Factors
If you have the following lifestyle habits, it may increase your risk of intestinal cancer [7].
- High fat diet
- Diet that is high in red meats, sodium, and smoked food.
- Smoking
- Excessive alcohol intake
Health History Factors
Should you have a history of the following conditions, it may increase your risk of intestinal cancer [8].
Crohn Disease — a chronic inflammation of the digestive tract. If you have Crohn Disease, you have a higher risk of developing both intestinal cancer (Adenocarcinomas) and colorectal cancer. However, only 2% of people with Crohn Disease will develop intestinal cancer [7].
Celiac Disease — a digestive disease that causes an obstruction in the absorption of nutrients in the small intestine. Celiac disease is an autoimmune disorder that prevents the consumption of gluten as it will damage the small intestine [9].
Familial Adenomatous Polyposis (FAP) — a genetic condition that causes the growth of many polyps (hundreds to thousands) in our bowel lining. if left untreated, there is a high chance that these polyps may become cancerous. People with FAP also have a higher risk of developing other types of cancer such as stomach cancer, thyroid cancer and pancreatic cancer.
**Lynch Syndrome — also known as hereditary non-polyposis colorectal cancer (HNPCC), Lynch Syndrome is a genetic disorder that predisposes an individual to different types of cancer such as intestinal cancer, colorectal cancer, stomach cancer, and many more [10].
**Peutz Jeghers Syndrome — a genetic condition where non-cancerous polyps form in the digestive tract. Patients with this syndrome are 15 times more likely to develop intestinal cancer as compared to the general population [11].
Is Intestinal Cancer curable?
As of today, Intestinal cancer is curable with the help of surgery. However, there are several factors that affect your chances of recovery. These factors are:
- The type of small intestine cancer (Adenocarcinoma, Sarcoma, Carcinoid Tumours, Lymphoma)
- Whether the cancer is localised or has spread beyond the walls of the small intestine
- Whether the cancer has spread to other places in the body (e.g. lymph nodes, liver etc).
- Whether the cancer can be eliminated completely with the help of surgery.
- Whether it is a newly diagnosed cancer or a recurring cancer.
Generally, the earlier you detect the cancer, the higher the chances of successful treatment.
Every patient is different. It is important that you communicate with your doctor to devise a personalised treatment plan for your condition. We will be exploring the various treatment options further down the article.
What is the survival rate for Intestinal Cancer?
We will be looking at the survival rate for intestinal cancer based on a 5-year timeline after diagnosis. I will be grouping them based on how far the cancer has spread at the time of diagnosis [12].
Stage
Survival Rate
Localised — the cancer is still within the walls of the small intestine.
86%
Regional — the cancer has spread to nearby areas or the lymph nodes.
76%
Distant — the cancer has spread to areas of the body that are far away from the small intestine (e.g. liver).
42%
As mentioned earlier, every patient is different. These numbers are only an estimate and you should not live by these numbers. However, it will help you get a better understanding of the success rates of your current treatments.
How is Intestinal Cancer diagnosed?
There are several tests and procedures that doctors use to either:
- Detect Intestinal cancer
- Diagnose Intestinal cancer
- Stage Intestinal cancer
The performance and results of these tests are important for your doctor to do any subsequent treatment planning.
Before any real testing, your doctor will go through the basic physical examination and history taking. The physical health examination helps to check for:
- General signs of health
- Signs of disease (e.g. unusual lumps)
Taking a complete history of your previous health conditions or lifestyle habits will allow your doctor to identify any potential risk factors of intestinal cancer.
Blood Tests
Should you be suspected of having intestinal cancer, your doctor may request for a blood test to be done. The blood test will measure:
Your complete blood count (CBC) — this measures your level of red blood cells, white blood cells and platelets. This is because intestinal cancer may cause bleeding in the small intestine. This can result in a low red blood cell count (anemia) [13].
Liver function tests — this helps determine if there are any signs of liver disease that may be a result of intestinal cancer.
Endoscopy
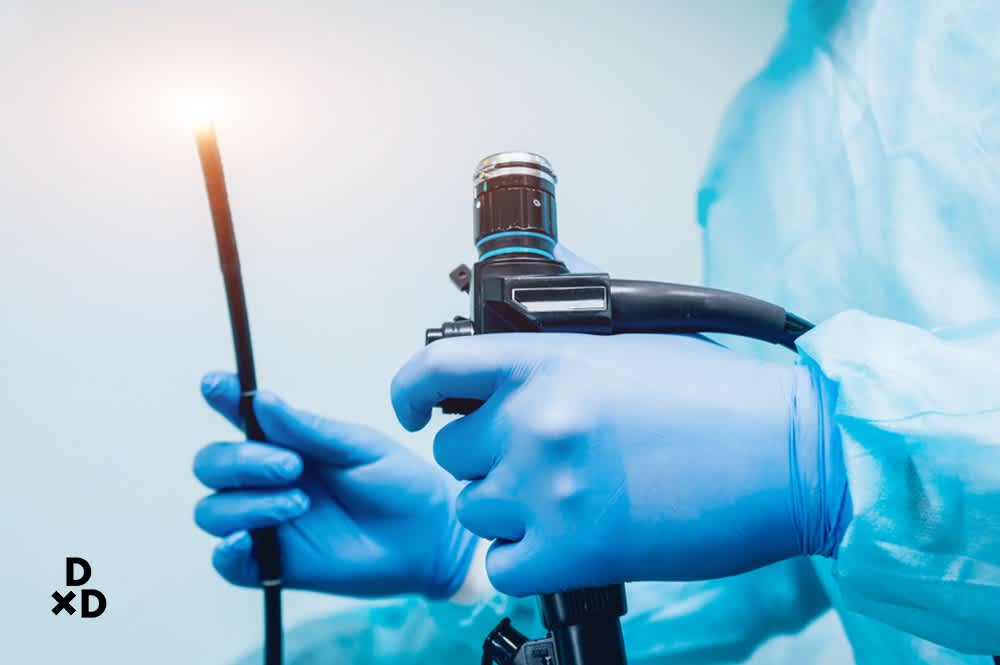
Your doctor may also require you to undergo an endoscopy in order to directly examine the inner lining of your digestive tract. Should any abnormalities be present, a piece of that area can be extracted for a biopsy.
Depending on the part of the small intestine, there are different types of endoscopy procedures that your doctor can perform:
Upper Endoscopy
This helps to look at the inside of your oesophagus, stomach and duodenum (the first part of your small intestine, closest to your stomach). The endoscope (a thin, tube-like instrument) is inserted through your mouth. It then passes through our oesophagus and into the duodenum.You will be given a local anaesthetic spray to numb the throat area and an option of a sedative injection that will help you relax during the endoscopy. However, should you choose to have the sedative, you will need to:
stay in the hospital for a longer time
arrange for someone to pick you up from the hospital
Have someone physically present for the next 24 hours
Capsule Endoscopy
Instead of using an endoscope, this procedure instead requires you to swallow a capsule that has a light and camera function within it. The capsule will travel through your stomach and small intestine while taking thousands of pictures in the process. This process usually takes around 8 hours.Images from the camera will be sent to a device that you will be wearing around your waist as you go about your daily routine. Your doctor views the collection of pictures to detect any signs of cancer.
For those of you wondering — what happens to the capsule then? Fret not, it will be passed out of your body during your usual bowel movement!
Double Balloon Endoscopy
A double balloon endoscopy is needed as the upper endoscopy is not able to view the entire small intestine.Just as the name suggests, a double balloon endoscopy uses a special endoscope that is made up of 2 tubes with one inside the other. Depending on the part of the small intestine that your doctor wishes to look at, the endoscope is inserted either through the mouth or the anus [14].
Once it has entered your small intestine, the inner tube of the endoscope that has a light and lens for viewing is pushed forward and a balloon at the end is inflated to anchor it. The outer tube is then also pushed forward and similarly, it is anchored in place with a balloon. The entire process repeats itself, thereby allowing the doctor to see the entire small intestine one foot at a time. Should any abnormality be detected, the doctor can then extract a piece of the tissue for biopsy.
Double balloon endoscopy is usually used to retrieve tissue samples for biopsy if the results from the capsule endoscopy shows signs of abnormality [13].
CT Scan
In a CT scan, x-rays are used to create highly detailed cross-sectional images of our body. It is able to see details on a tissue-level as opposed to a regular x-ray.
Your doctor will usually recommend a CT scan if you have symptoms of abdominal pain [13]. However, CT scans are not the best at identifying small intestinal tumours but are useful for determining the problems that arise as a result of the tumours.
They are also useful tools for finding the areas where the cancer cells have spread to.
Magnetic Resonance Imaging (MRI)
While a CT scan uses x-rays, and MRI uses radio waves and strong magnets [13]
The picture created from an MRI is much more detailed as compared to a CT scan. Hence your doctor might recommend an MRI if he suspects that you have tumours in your small intestine [13].
Biopsy
Regardless of the type of cancer, a biopsy is the only concrete way for a doctor to know if an area of the body has cancer.
During your biopsy, your doctor extracts a sample of tissue of the suspected area and has it tested in a laboratory. The results of your biopsy should be ready within 1-2 days.
Biopsies can be done through an endoscopic procedure or with the use of an imaging-guided fine needle apparatus. If the suspected area is inaccessible by those methods, surgery is required to obtain the sample. [13]
What can I expect during my first consultation?
Receiving news about a positive cancer diagnosis is certainly not an easy pill to swallow. There are a lot of unknown factors that you as a patient have to face together with your doctor.

In the first consultation, your doctor would talk about the options for treatment. Each treatment option would vary in efficacy and may have various side effects.
Thereafter, your doctor would possibly advise on a recommended course of treatment. Your doctor would ensure that you understand the journey you are about to take to recovery.
How is Intestinal Cancer treated?
The recommended treatment options available for intestinal cancer may vary on many different factors as no two tumours are the same.
As with any type of cancer condition, while there are standard treatment options that are available to cancer patients, clinical trials that are research studies testing on new therapies may also be considered.
Generally, the treatment options for intestinal cancer may depend on [15]:
- Resectability
If the tumour can be removed via surgery - Extent of cancerIf the cancer is primary or metastatic (spread)
- Extent of cancerIf the cancer event is not the first
Treatment options for the different types of intestinal cancer
The following segment contains the main treatment options for each type of intestinal cancer based on their resectability, extent of cancer and if the cancer is a recurred event. [15]
Adenocarcinoma
Standard treatment options for adenocarcinoma include [15]:
- Resectable primary disease
Radical surgical resection may be considered. It involves surgically removing the tumour or mass.
- Unresectable primary disease
A surgical bypass of the tumour, if it is obstructing the small intestinal, can be conducted. The condition is unresectable which means the tumour may not be able to be removed but the parts of the small intestine may be redirected through surgical bypass to re-establish clear passage of the digestive tract. [16]
Palliative radiation therapy is another option which involves the use of low doses of high energy X-rays to the affected area in the aim to help alleviate the symptoms of the disease. [17]
Treatment options used in clinical trials include:
- Unresectable primary disease
Radiation therapy methods under clinical evaluation can be considered. They target the primary area affected with the use of compounds that cause tumour cells to be more vulnerable to radiation. [18] It can be done with or without systemic chemotherapy.
- Unresectable metastatic disease
New drugs and therapeutic agents that are still being researched on in clinical trials can be considered. [15]
Sarcoma
The standard treatment options to consider for sarcomas such as leiomyosarcoma and GISTs include:
- Resectable primary disease
Radical surgical resection can be done. [15]
- Unresectable primary disease
Surgical bypass of obstructing lesion and radiation therapy are possible options. [15]
Some large tumours may require chemotherapy with the use of imatinib which helps to shrink the tumour. If the size of the tumour is reduced sufficiently, surgery can be done. [19]
- Unresectable metastatic disease
Some procedures can be done to help alleviate the symptoms and can be done through palliative surgery, radiation therapy and chemotherapy. [19]
Treatment options used in clinical trials include:
- Both types of unresectable diseases
New drugs and therapeutic agents under clinical evaluation can be considered.
Recurrent intestinal cancer conditions
The treatment options for recurrent cancers are similar between adenocarcinoma and sarcoma conditions.
- Recurrent metastatic disease
The use of new drugs and therapeutic agents still being researched in clinical trials should be considered in this case. [15]
- Recurrent primary disease
Similar to aforementioned options, surgery, palliative radiation therapy and palliative chemotherapy. [15]
What can I expect during treatment?
**Surgery
Surgery for intestinal cancer would involve the use of anaesthesia to ensure that you do not feel pain during the procedure. Depending on the size of the cancer formation, the surgery may be minimally-invasive through laparoscopy or open surgery which would involve a large cut in the skin. [20]Resection surgery for adenocarcinoma involves removing the tumour-affected part of the intestine and rejoining the 2 cut ends of the small intestine. For tumours in the ileum, the first part of the large intestine may be removed along as well. [16]
A few days may be required post-surgery before the patient can eat and drink properly. [16]**
**Radiotherapy
The team of specialists helping to administer your radiotherapy would firstly derive important measurements through imaging tests pre-treatment so as to calibrate their radiotherapy apparatus properly. This includes obtaining the optimum angle and the correct dose of radiation. [21]Most of the time is spent on the pre-treatment tests while administering the radiotherapy would only take a few minutes. Daily weekday sessions may be required for a few weeks to a few months. [22]** You may experience side effects such as fatigue, nausea, diarrhea or localised skin conditions. [22]
**Chemotherapy
Drugs are used to target the tumour cells. They can be administered through an intravenous (IV) needle through the arm or through orally through pills.You may experience similar side effects to radiotherapy and also loss of appetite, hair or mouth sores additionally. [23]**
Will I be required to stay in the hospital?

Depending on certain factors, such as the type of cancer and treatment, you may or may not be hospitalised. For example, you can expect to be hospitalised if a surgery is performed. Conversely, chemotherapy and radiotherapy may not require hospital stay.
What is the cost of treatment for Intestinal Cancer?
Based on information provided on Ministry of Health’s website, the majority of the cost of treatment for intestinal cancer falls within the following ranges:
Public Hospitals/Centres (Subsidised) Up to about $2,800
Public Hospitals/Centres (Unsubsidised) Up to about $5,700
Private Hospitals/Clinics Up to about $16,000
How much of this is Medisave claimable?
For surgical operations, the amount withdrawable from Medisave follows the categorisation of the operations in the Table of Operations. [24]
Table of Operations
Medisave Withdrawal limits
1A - 1C
S$250 - S$450
2A - 2C
S$600 - S$950
3A - 3C
S$1250 - S$1850
4A - 4C
S$2150 - S$2850
5A - 5C
S$3150 - S$3950
6A - 6C
S$4650 - S$5650
7A - 7C
S$6200 - S$7550
Most surgical operations pertaining to cancerous growths fall in the 4A-7C categories and so the range of withdrawal limits should be $2,150-$7,550, depending on the operation.
Most of the outpatient treatments that are Medisave claimable are as shown below: [24]
Type of treatment
Medisave Withdrawal limits
Outpatient imaging scans such as MRI and CT
Up to $600 per year per patient
Chemotherapy
$1,200 per month per patient
External radiotherapy
$80 per treatment
Brachytherapy with external radiotherapy
$300 per treatment
Brachytherapy without external radiotherapy
$360 per treatment
Superficial X-ray
$30 per treatment
**
Is this inclusive of palliative care?**
For home palliative care or day hospice care, the Medisave Withdrawal limit is $2,500 per patient’s lifetime. [25]
What can I expect post-treatment?
After the main treatment regime has been completed, patients may still have to undergo follow-up care. This includes regular physical examinations and medical tests so that the doctors can monitor your recovery as time goes by. [26]
A key objective of follow-up care is to detect recurrences which may be possible.
Are there any lifestyle changes after Intestinal Cancer treatment?
Depending on the treatment received for the patient’s cancer condition in the past, there may be long-term side effects that have not subsided. These may be physical or emotional in nature.
It is paramount that you are able to discuss your worries and concerns with your doctor, so that they can help ensure that you are able to manage these issues in the long run. [26]
What can I do to prevent Intestinal Cancer?
You can only make a conscious effort to lead a healthier lifestyle and avoid specific habits and dietary choices to reduce your risk of intestinal cancer.
These include:
- Smoking
- Alcohol
- Eating too much red meats
Conclusion
Knowing more about intestinal cancer may alleviate some of your worries but speaking to your trusted doctor about it would ensure that you get the best care and treatment options possible.
Head over to general surgeon, Dr Ravishankar’s profile to book a consultation.